‘Young doctors are planning funerals — their own. They are intubating patients — their colleagues. And they are hearing bedside monitors beep and fall flat over and over again in a single shift, only to return to more of the same in the next shift, and the next, as they find their years of training unequal to the awful challenges of the covid-19 pandemic.
Last month, a prominent Manhattan emergency room doctor, Lorna Breen, died by suicide after describing the horrific events she had witnessed while fighting the disease caused by the novel coronavirus. Her death highlighted what some of us in the mental health community have known since the start of the crisis: that the psychological impact of what is happening in American hospitals will stay with us long after the immediate crisis subsides and that among those most affected will be health-care workers. All agree that we should focus on how to help them seek the care they may need, but little has been said about the barriers that can discourage them from reaching out — or that a significant barrier is medical licensing.
The pandemic has provoked fear in doctors and nurses. They’re scared, not just because they so often can’t save the lives of covid-19 patients, but because they can’t always protect themselves and their families from infection. Those like Breen who lead a hospital department probably feel most the additional burden of having to keep their colleagues safe and fight for protective equipment. National shortages, coupled with the highly contagious nature of this virus, have resulted in workers and vulnerable relatives getting sick and, in some cases, dying. No doctor imagines having to treat a colleague; confronting our own mortality and safety in the workplace on a daily basis is something none of us were taught in medical school. It makes the mundane experience of going to work terrifying and even traumatic.
The toll that trauma and post-traumatic stress puts on the body is well-established. We’ve also known for some time that trauma can change the structure and chemical makeup of the brain. It hijacks the brain’s ability to reason and activates our most primal emotional responses. It should come as no surprise, then, that there is a proven link between trauma and suicide. While we do not know the specific circumstances of Breen’s challenges — she had also contracted the virus herself — we do know that her experience in the hospital, as relayed by her father and sisterin the news media, is the experience of countless other health-care workers who remain on the front lines and, consequently, face the same risk. The common symptoms of trauma include avoidance of reminders of the traumatic event, nightmares with similar themes, flashbacks and intrusive memories, critical self-evaluation, guilt, negative mood, anxiety, panic attacks and detachment or dissociation. When these symptoms go untreated, sufferers become vulnerable to post-traumatic stress disorder (PTSD), other serious disorders and, yes, suicide.
Early treatment is essential to the prevention of a potentially debilitating, if not deadly, outcome, but physicians, in particular, face elevated levels of scrutiny when disclosing any form of mental health treatment to state licensing boards. For many doctors, the repercussions they may face introduce a significant obstacle. About 90 percent of state licensing applications include a question about a physician’s mental health, and some even ask questions about past diagnoses, such as depression or anxiety, that may have occurred before medical school. This goes against the recommendation of the American Medical Association and has been cited in studies as a significant reason that physicians are reluctant to seek mental health care.
Although there is no reason to believe that psychiatric diagnosis or treatment poses a risk to patients unless the physician has very serious ongoing symptoms, answering yes to these questions often leads to further questions. The state licensing board can require all of your medical and mental health records, including intimate details about your upbringing, your family and your spouse that you may have divulged in private psychotherapy sessions. Your license may be contingent upon sharing these records.
Moreover, after sharing your records, the board can then dictate further evaluation and possibly send a physician to a Physician Health Program (PHP). Initially started to assist physicians through tough times, some PHPs have earned a poor and even malignant reputation over the years, partly because they have financial arrangements with select institutions across the country. PHPs reportedly send physicians to these institutions — at their own expense — for costly cash-only evaluations that sometimes last several weeks. After the evaluation, the PHP may require supervision of the physician’s practice of medicine, a workplace monitor whose job it is to report back to the PHP about the “troubled physician,” or order random check-ins even without any specific evidence of current impairment.
Once a PHP requires this evaluation, the physician is trapped. If you don’t enter into a contract with the PHP to fulfill whatever requirements have been outlined, you risk permanently losing your medical license. Many physicians caught in what some believe to be a corrupt PHP system have written about their experiences, and others who know how this system works have advocated for these doctors, but PHPs still exist and physicians still fear them…’




/cdn.vox-cdn.com/uploads/chorus_image/image/66877991/GettyImages_1216479484.0.jpg)


/cdn.vox-cdn.com/uploads/chorus_image/image/66861002/1211871002.jpg.0.jpg)

/cdn.vox-cdn.com/uploads/chorus_image/image/66839623/GettyImages_1224708188.0.jpg)




 ‘In November 2019 — six months ago this week — Trump began what the White House described as “portions” of his third physical during a two-hour examination at Walter Reed National Military Medical Center.
‘In November 2019 — six months ago this week — Trump began what the White House described as “portions” of his third physical during a two-hour examination at Walter Reed National Military Medical Center.
/cdn.vox-cdn.com/uploads/chorus_image/image/66831294/1213411124.jpg.0.jpg)

:no_upscale()/cdn.vox-cdn.com/uploads/chorus_asset/file/19990665/download.jpeg)
 The press touts a coronavirus milestone as the global count passes 5 million. Of course, the count bears the same relationship to the realities as Plato’s shadows on the cave wall. Alex Madrigal in The Atlantic
The press touts a coronavirus milestone as the global count passes 5 million. Of course, the count bears the same relationship to the realities as Plato’s shadows on the cave wall. Alex Madrigal in The Atlantic 





/cdn.vox-cdn.com/uploads/chorus_image/image/66801792/GettyImages_1224248234.0.jpg)


 Literary scholar Elizabeth Outka finds the pandemic between the lines in literature.:
Literary scholar Elizabeth Outka finds the pandemic between the lines in literature.:

/cdn.vox-cdn.com/uploads/chorus_image/image/66769671/GettyImages_1175977697.0.jpg)

 The new study, reported in StatNews,
The new study, reported in StatNews, 
 Things did not end well for him.
Things did not end well for him.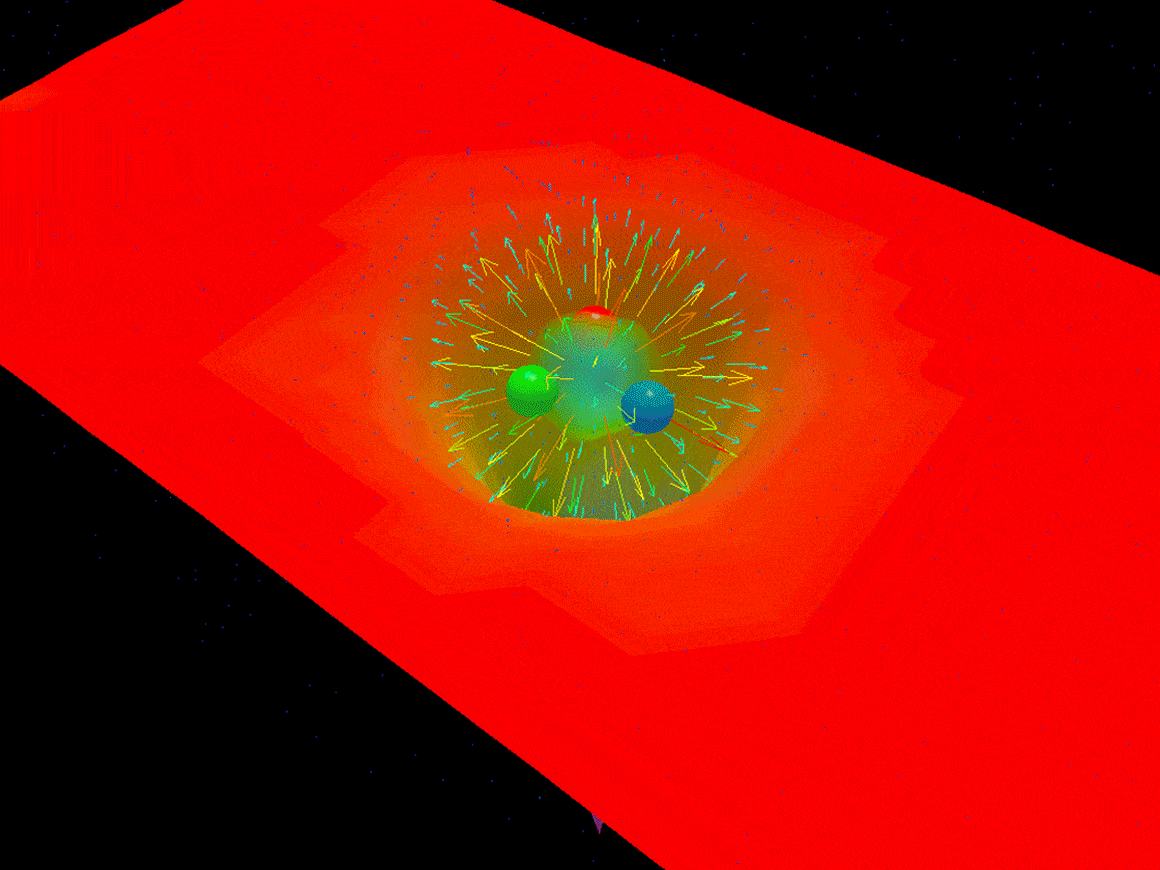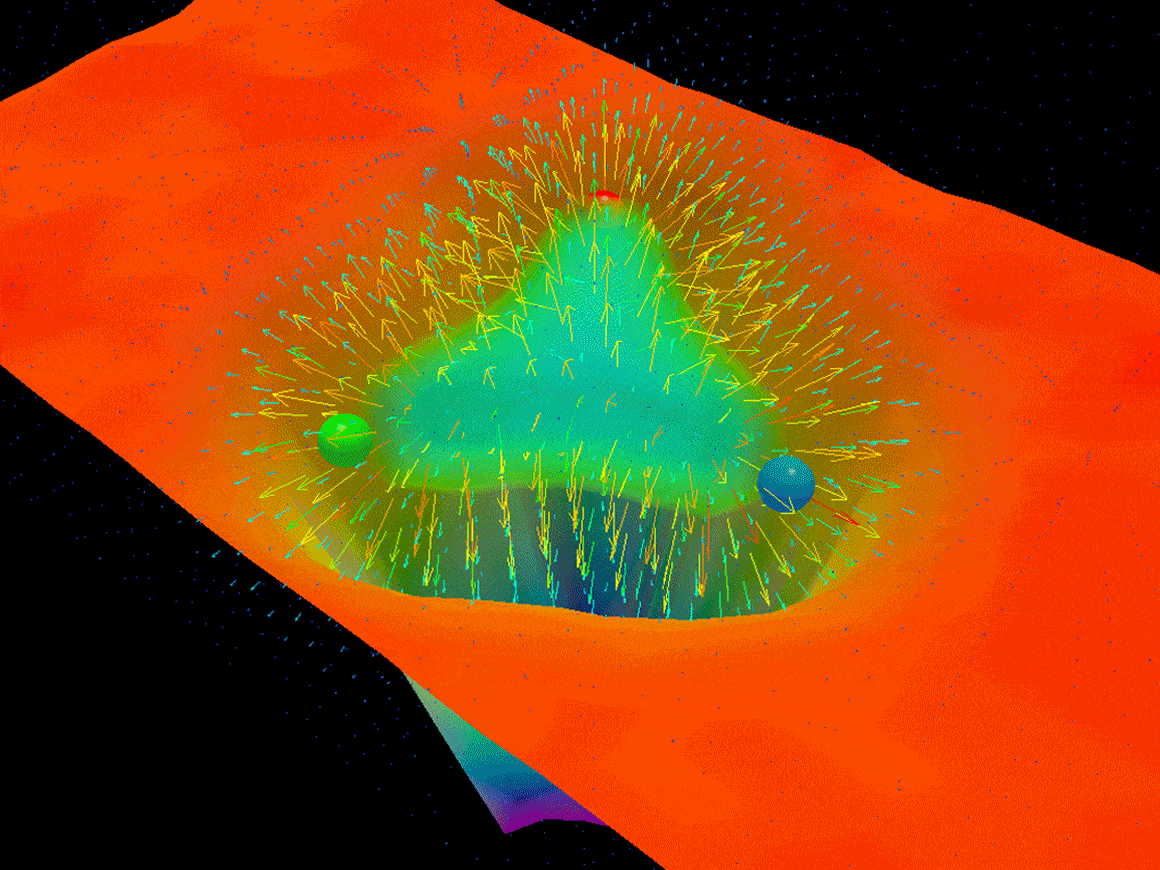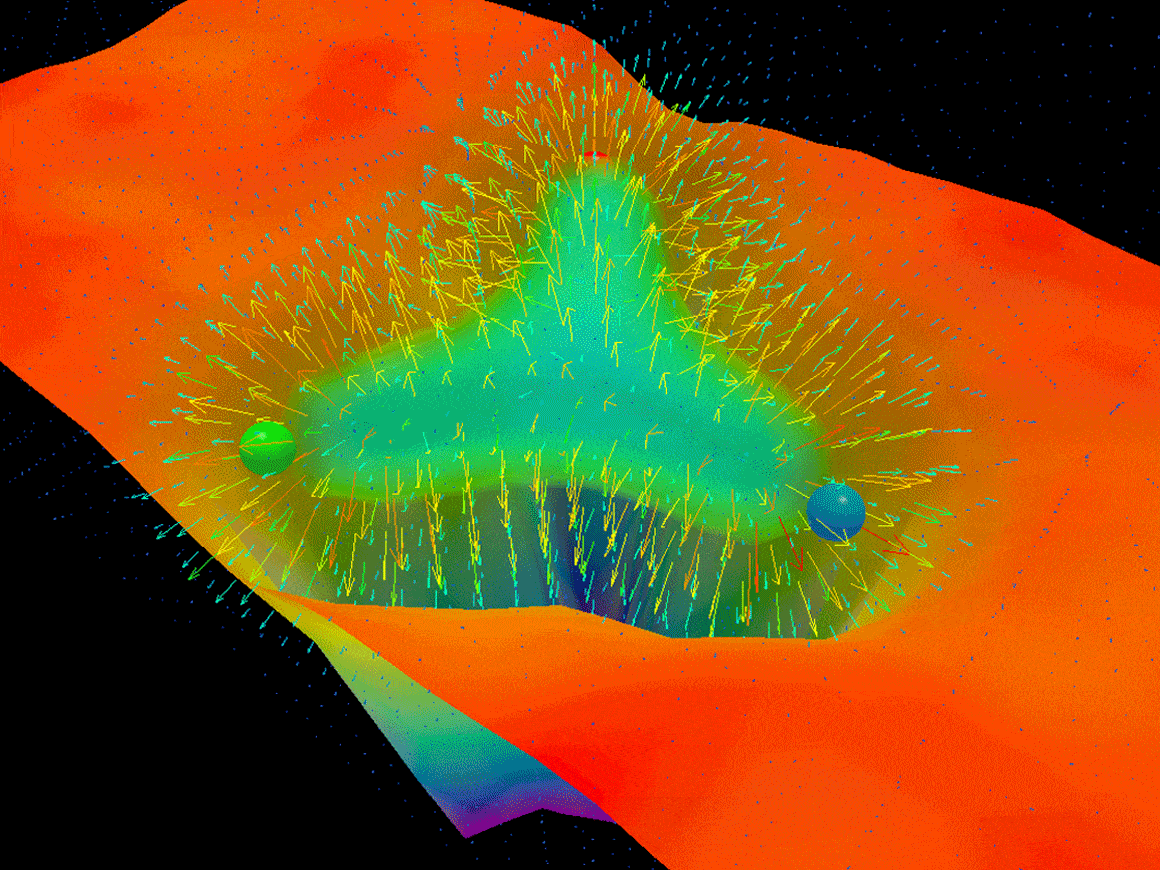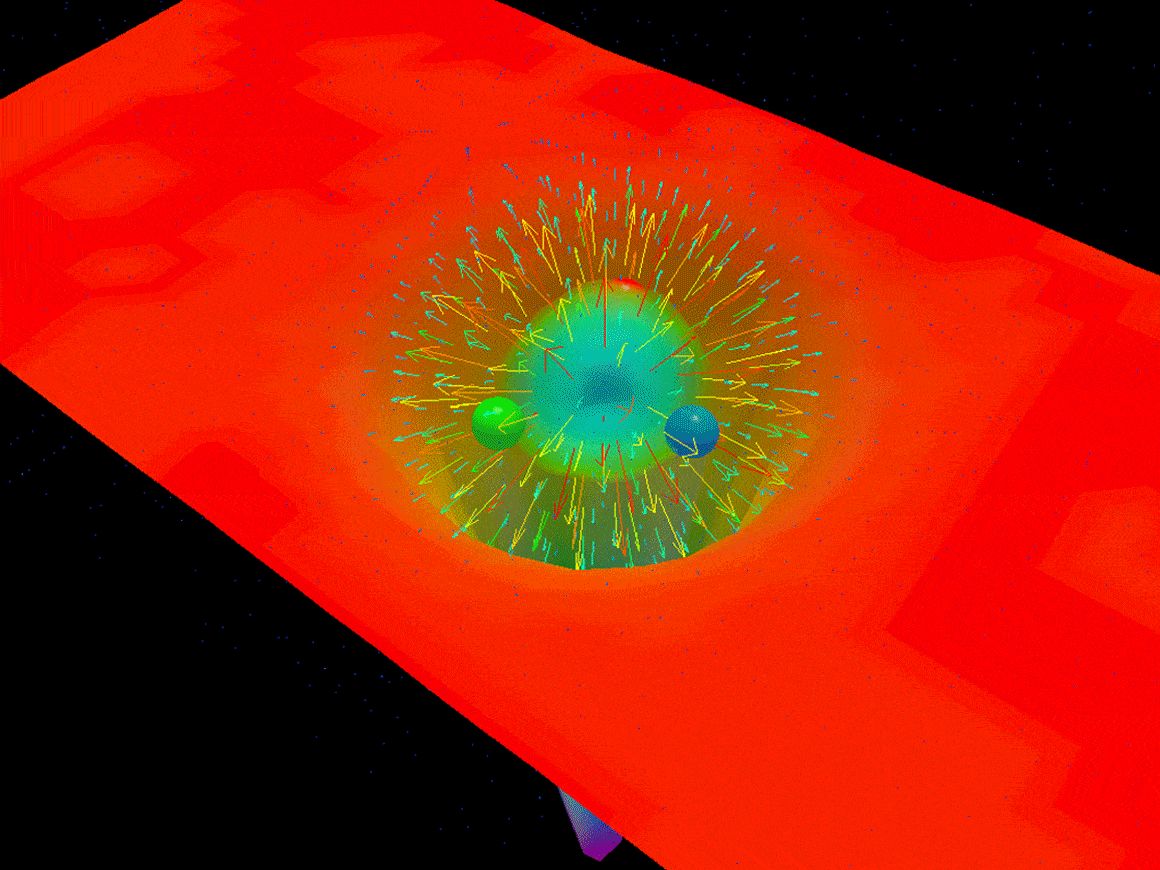 Objects are made of atoms, and atoms are likewise the sum of their parts — electrons, protons and neutrons. Dive into one of those protons or neutrons, however, and things get weird. Three particles called quarks ricochet back and forth at nearly the speed of light, snapped back by interconnected strings of particles called gluons. Bizarrely, the proton’s mass must somehow arise from the energy of the stretchy gluon strings, since quarks weigh very little and gluons nothing at all.
Objects are made of atoms, and atoms are likewise the sum of their parts — electrons, protons and neutrons. Dive into one of those protons or neutrons, however, and things get weird. Three particles called quarks ricochet back and forth at nearly the speed of light, snapped back by interconnected strings of particles called gluons. Bizarrely, the proton’s mass must somehow arise from the energy of the stretchy gluon strings, since quarks weigh very little and gluons nothing at all. Republicans broadly agree that mass deaths are an acceptable sacrifice in the effort to “reopen” an economy savaged by the coronavirus pandemic. This approach got its media moment yesterday as Trump toured a mask factory to Paul McCartney’s classic hit Live and Let Die.
Republicans broadly agree that mass deaths are an acceptable sacrifice in the effort to “reopen” an economy savaged by the coronavirus pandemic. This approach got its media moment yesterday as Trump toured a mask factory to Paul McCartney’s classic hit Live and Let Die. ‘In this essay, Roy Scranton asks what we mean when we say “the world is ending.” Examining the nature of the narratives we tell ourselves about the future, he explores what revelation may be before us.
‘In this essay, Roy Scranton asks what we mean when we say “the world is ending.” Examining the nature of the narratives we tell ourselves about the future, he explores what revelation may be before us.

/cdn.vox-cdn.com/uploads/chorus_image/image/66747370/yoCKYEIg.0.jpeg)
