
US licensing of esketamine, a version of the drug ketamine, “could usher in a wave of fast-acting treatments, but experts are worried.”
As a clinical psychiatrist, wrestling with the treatment of severe resistant depressive conditions in my patients, I share some of the concerns about possible side effects, long-term risks and potential associated social ills raised in this Guardian article.
Ketamine has a broad range of brain effects. It is a euphoriant, a hallucinogen, a dissociant, and an anaesthetic in overlapping but different dosage ranges. The article quotes Dr Carlos Zarate, head of experimental therapeutics and pathophysiology at the US National Institute of Mental Health, who conducted the first clinical trial of ketamine for depression in 2006, who says, in part,
“What’s particularly interesting about ketamine is that it has multiple effects throughout different brain biologies… This makes it much more unique than other treatments. Many of the symptom domains seen in depression, but not all, seem to respond to it.”
Zarate and other prominent psychiatrists can perhaps be forgiven for their enthusiasm for what they describe as the first truly novel development in the drug treatment of depression in several decades. However, let’s look at what I see as the absurdity in this comment. ‘Depression’ is a catchall name for biologically diverse conditions and states of mind, and increasingly so in the past few decades as manufacturers have marketed the expansion of the term in order to expand demand for their antidepressant products. Ketamine is far from ‘unique’ in its nonspecificity! If it acts immediately and acts across a range of depressive types and symptoms, it is fairly certain that it is not addressing the underlying pathophysiology of the condition but rather providing a generic ‘feel-good’ effect. To mix metaphors, it is sort of like using a sledge hammer to drive in a thumb tack… and, if it’s the only tool you’ve got, then it pays to see everything as if it is a thumb tack, right? (Certainly, those who sell sledge hammers would have you see it that way!)
Any drug with nonspecific euphoriant effects will make depressed people feel better. Indeed, they make anyone feel better. In this manner of speaking, cocaine and stimulant drugs (‘speed’) ‘treat’ depression. In fact, there is a school of thought (the ‘drug-of-choice’ model, or ‘self-medication hypothesis’) that some proportion of substance abuse patients may be unknowingly treating an underlying psychiatric disorder through their drug use. This extends to other intoxicants such as alcohol and sedative-hypnotics as well. Using nonspecific euphoriants for their antidepressant effects causes immense problems, and the use of ketamine may fall into that category.
The first of these is potential tolerance. This refers to the fact that the brain inures itself over time to the effects of the substance. It is not clear that ketamine will cause physiological tolerance — and there have not been long-enough duration studies to tell — but it is certainly possible. The brain resists being pushed out of its usual range of functioning into a euphoric state. With increasing resistance, it takes more and more of the substance, or more and more frequent administration, to produce the desired effect. One will be chasing one’s tail, so to speak, in a vicious cycle — the more one uses, the more one needs. There may come to be less and less therapeutic benefit or benefit only at such dosage that toxic effects start to predominate. To maintain its antidepressant effect, current guidelines suggest a weekly interval for esketamine treatment. Given the chronicity of some depressive conditions, patients may need to continue treatment over a period of years or even indefinitely. Dosages may need to be higher or treatments more frequent as time goes on. One could imagine that the pharmaceutical industry would welcome such captive audiences requiring open-ended treatment modalities.
Closely related to the development of tolerance is the potential for dependency. Ketamine is probably not physiologically dependency-inducing (“addictive”), in the sense of needing to keep using it to stave off physiological withdrawal (“drug sickness”) upon cessation. But a substance that makes people feel good so quickly is highly reinforcing and may thus be psychologically addictive even if not physically.
Proponents point out that the benefits of treatment may outweigh the risks for patients who have no other options. This begs the question of whether its use will continue to be restricted to patients whose depression is treatment-resistant and has failed other available options. After all, the last innovation in antidepressant development, the introduction of the SSRIs (Prozac and its cousins) in the 1980’s was originally meant to rescue those whose depression was resistant to the treatments of the day (the tricyclics and monoamine oxidase inhibitors). Now they have become the first-line treatments, completely supplanting the older agents in modern psychiatric practice… and some argue that they are inferior antidepressant agents for clinically significant clinical depression. To call them good antidepressants, society has had to accept a vastly expanded definition of depression. This loss of linguistic precision contributes to the ongoing medicalization of everyday life problems, to our detriment.
(I’m talking about the circular reasoning pitfall here. If someone’depression seems happier on ketamine, then ketamine is having an antidepressant effect. And if it is seen as an antidepressant, then anyone who responds to it had depression. And so on.)
I share the misgivings of Dr. Julie Zito, professor of pharmacy and psychiatry at the University of Maryland, who sums it up:
“There’s been a huge expansion in what constitutes depression. There are low-moderate depressives who are going through a divorce or struggling with a new job… What they might really need is counselling. But in the US, we love our pills and simple solutions to very complex problems.”
A further complication of esketamine use may be that, once available in the marketplace, we may be unable to stem its diversion for street use, either for recreational use or unsupervised self-medication for self-diagnosed depression. After all, we haven’t done such a great job with prescription opiates, and it does not appear we have learned much from that.
It is also important to recognize that esketamine was approved after only four relatively small and short-lived clinical trials with decidedly mixed results. As Zito points out,
“The FDA created this new innovative study category, which means they only required one randomised, double-blind placebo-controlled trial, not two, which is usually the criterion for a new drug.”
Furthermore, not only the breadth or duration of the drug’s benefit but its depth are in question. A treatment may be found to be superior to placebo in the sense of demonstrating a statistical toy significant difference on an outcome measure in a clinical trial, but this may not translate into something clinically meaningful to the patient’s life. In other words, this may not be a distinction that makes a difference. Such logically fallacious conclusions are a generic problem in psychopharmacological research. Zito, again, on the ketamine trials:
“They evaluated the efficacy using symptom score change and there was only a three- to four-point improvement on a 60-point scale, which you have to say is very modest. And that is what the whole thing hangs on.”
In the absence of robust and extensive double blind placebo-controlled trials, the interest in ketamine relies heavily, then, on anecdotal and first-person accounts of dramatic improvement. The benefits may derive from suggestion effects — a substance that drastically alters consciousness or subjective experience, as ketamine does, is a strong candidate to mobilize the placebo response, inspiring in the recipient the self-fulfilling prophecy that it is having a powerful effect. I am not entirely scoffing about this; I believe that a good part of the effect of many of the medications we use arises from enlisting the patient in a belief system in which the medication is helping, thus mobilizing their self-healing.
Concerns have repeatedly been raised about effects of ketamine administration such as hallucinations, out-of-body experiences, and fluctuations in blood pressure. Patients receiving esketamine will be required to remain in the clinic or the doctor’s office for two hours of monitoring after each treatment. But people are different; who is to say that someone will be free of risk precisely at the two-hour point? In preapproval studies, there were three suicides in the esketamine group as well as a fourth death in which a patient crashed his motorcycle shortly after dosing. (Hard to say, but did that represent suicidal intent? Impairment of judgment? Or perceptual and coordination problems?)
Of course, the manufacturer asserts that all those events were unrelated to the actions of the drug, but there were no corresponding events in the placebo group. With such a small studied group, certainly this difference may have been statistical accident, and severe depression indubitably carries suicide risk. But there have also been concerns about exacerbation of suicidal tendencies with earlier antidepressants. Going into detail about this concern is the subject for a different essay, but I’ll mention several different potential dangerous mechanisms. First, any side effects that make a person more uncomfortable (e.g. the restlessness and agitation caused by several of the SSRIs) can be the straw that breaks the camel’s back, tipping them over the edge to decide not to endure discomfort any longer. Second, not all symptoms of depression respond to treatment at the same rate. If a person’s depressive lack of energy and paralysis of will improve before their despair does, their motivation to act on their despondency may be mobilized. Third, some drugs, and ketamine as a euphoriant may be among them, may act by lowering inhibitions, including control over latent self-destructive urges.
Advocates of the use of ketamine and esketamine, thus, may be ignoring the fact that the Emperor has no clothes. We know too little about the pathophysiology of depression and too little about the pharmacology of ketamine. Classically, exposition on antidepressants has relied on the ‘monoamine hypothesis’ for the illness and the fact that the drugs address monoamine (primarily norepinephrine and serotonin) deficits. Yet, that has clearly been an incomplete or inadequate explanation. More recently, the focus in depression and just about every other psychiatric condition has turned to a different neurotransmitter, glutamate. There’s a lot of handwaving but we do not have a precise or coherent understanding of how glutamate is implicated in the mechanism of various disorders; certainly nothing that would guide clinical practice. And, surely enough, ketamine is thought of, among other actions, as a glutamate receptor blocker. Post hoc ergo propter hoc?
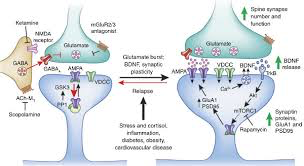
Similarly, in this post-monoamine world, there is a lot of handwaving interest in the idea that depression treatments may also work by correcting physical damage to nerve cells implicated in depression. Sure enough, the article invokes this ‘neuromythology’:
“…one idea is that (ketamine) triggers the brain to regrow connections between cells that are involved in mood, but no one really knows for sure.”
A complicated set of misgivings. In short, let us hope that ketamine, through its hallucinogenic effect, is not causing us to hallucinate clothes on the Emperor.


One of your best posts, ever !
LikeLike